What is Piles?
When the pressure on the veins in the rectal region increases, they swell. These swellings resemble a bag of worms and refer to as Piles or Haemorrhoids. The term Haemorrhoids is more used in the American continent. Piles or Hemorrhoid is also the ultimate penalty we pay as a result of our evolution that has made us walk upright.
More About Piles or Haemorrhoids
Types of Piles
There are two types of piles, namely, internal piles and external piles. Internal piles are more common than external piles.
Internal Piles
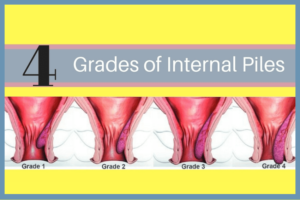
When this swelling is present internally within the anus, on the anal lining, they are termed as internal piles. They form slightly above a line called the dentate line or pectinate line. The entire anal canal is divided into an upper two-third portion and a lower one-third portion by this dentate or pectinate line. They precisely form between 2 and 4 centimeters above the anal opening. There are four grades of Internal Piles.
External Piles
When this swelling is present externally outside the anus, precisely beneath the skin that surrounds the anus, they are termed as external piles.
Grade-1 Internal Piles
The piles condition is fresh and asymptomatic and is present internally above the pectinate line. Pain does not manifest at this budding grade of piles. Just that the veins that are facing the intense pressure are beginning to show symptoms of piles. The patient rarely feels discomfort at this stage. Some patients might experience itching and discomfort
Grade-2 Internal Piles
The piles condition begins to experience something called “prolapsed”. Prolapse is nothing but the veins becoming weak and beginning to move out of the anal canal. The secondary grade piles condition is painful. The prolapsed veins move up inside or reverse into the anal canal spontaneously. The patient feels discomfort and itching at this stage.
Grade-3 Internal Piles
This condition or grade is when the prolapsed veins become more painful and cause more discomfort because the spontaneous reversal or reduction of the prolapsed veins does not happen. However, the patient can manually push the prolapsed veins inside.
Grade-4 Internal Piles
This final condition or grade is where the prolapsed piles cannot be pushed inside the anal canal manually also. The piles hang outside and causes immense pain and discomfort.
Though internal piles are generically classified as per the above grades, the clinical classification based on what the Piles specialist or Proctologist observes can be classified rather differently. These can be called stages and each stage is characterized by how piles manifest further.
Clinical Classification of Four Stages of Internal Piles
Stage-1 Internal Piles
Proctoscopy shows that the piles veins occupy only less than 25% of the lumen.. Simply put, piles veins are beginning to appear to the piles surgeon upon observation.
Stage-2 Internal Piles
During the proctoscopy session with the patient, if the piles specialist observes that the lumen of the proctoscope is occupied 25% by the veins of piles, then it can be categorized as Stage-2.
Stages-3 Internal Piles
Similarly, if the lumen of the proctoscope is 50% occupied by the veins of piles during proctoscopy by piles specialist, then it is Stage-3. Additionally, the prolapse of the vein could be clearly observed by the piles surgeon and the surgeon could also confirm that the vein tuft automatically goes in.
Stages-4 Internal Piles
In this stage, the lumen of the proctoscope is completely accumulated by veins of piles. The prolapse of the vein also takes place and it needs to be pushed inside manually. In this stage, the veins cease to prolapse automatically inside.
Complicated Piles
The extreme end-stage of the internal piles is termed as complicated piles. The veins are fully thrombosed and are completely prolapsed. Manually pushing the veins inside is absolutely not possible in this stage and it is extremely painful for the patients at this stage.
Dr. Maran M on Internal Piles Classification
Dr. Maran, a Piles surgeon in Chennai treats piles and does piles surgery in Chennai regularly observes that if anyone has pain or any discomfort in the anal region, they have to immediately consult. If they see any droplet of blood in the stools it is best to consult a good Piles surgeon or a Proctologist. The diagnosis to rule out the cause for blood in the stool is absolutely necessary. Because sometimes it may not be piles or fissures, it can be something else also. So Dr. Maran always advises to take blood in stool with extra caution and suggests to visit a piles specialist sooner.
General Symptoms of Piles
(1) Spots of blood in the stool
(2) Pain when passing the stool. The pain can range from mild to severe depending on the severity of the piles.
(3) An itchy sensation around the anus.
(4) In severe cases of piles, a hard lump lies hanging from the anal region. This lump may be hanging externally or it can have its origin internally.
(5) A feeling of incomplete evacuation of stools.
Specific Symptoms of Internal Piles
(1) Often it starts as painless bleeding when passing stools. You can observe red spots of blood in your stools. The bleeding is not profuse or uncontrolled. It is just that it is present.
(2) In the next stage, when internal hemorrhoid swells, they can be felt like a lump outside the anus. They can be often pushed back inside.
(3) For the internal hemorrhoids that cannot be pushed back, they get stuck, and sometimes it swells even more. This stage requires immediate medical attention.
Specific Symptoms of External Piles
(1) There is a lump of tissue outside the anus. They are often painful and cause bleeding when passing stools.
(2) The tendency for hemorrhoids to develop swelling as it heals is high and this causes more pain.
(3) Increased pain can be felt as the patient with external piles sits or is seated in a toilet.
What is Prolapsed Piles?
The piles condition begins to experience something called “prolapsing”. Prolapse is nothing but the rectal mucosa along with the piles blood vessels projecting out are pushed outside the anal canal.
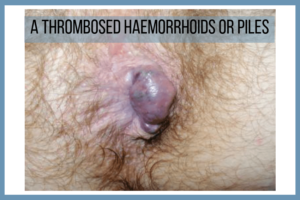
When blood clots inside the veins that have caused piles then they are referred to as thrombosed piles. A thrombosed piles does not have any blood flow due to the clot. They are very painfully though not dangerous. In most cases, it has been observed that thrombosed piles resolve themselves as the clot is reabsorbed by the body. Sometimes it does not and hence requires external intervention by the piles surgeon.
Causes of Piles
There are several factors that cause pressure on the veins in the rectal region. The various factors that cause this pressure are
(1) Constipation - Generally chronic constipation which has been around for quite a few years.
(2) Diarrhea – Chronic in nature
(3) Lifting heavy weights – This becomes a reason when a person uses improper lifting techniques while lifting any kind of weight. Gyms are not the only place where people lift weights. A bucket full of water, an LPG cylinder, lifting heavy machinery at work are some of the activities where lifting of weight takes place. Men do most weightlifting in the gym and in the workplace while women lift weights as they perform household chores.
(4) Abdominal Exercises – The exertion of pressure to the anal region when doing abdominal exercises is high and can lead to piles.
(4) Pregnancy – The growing fetus puts pressure on the abdomen cavity which in turn can cause the veins in the anus to swell. Also, women are more prone to constipation due to their pelvic shape. The instance of constipation increases during pregnancy which might also play a role.
(5) Straining while passing stools – This condition is closely tagged to constipation. Straining puts pressure on the veins and hence they are responsible for swelling of the veins in the anal region.
General Diagnosis of Piles
(1) A PIles Surgeon or a Proctologist is the one who does the diagnosis of piles or hemorrhoids. The surgeon initially questions the patients on the symptoms.
(2) The surgeon then proceeds for a physical examination of the anal region. Physical examination involves the surgeon wearing a glove, lubricating your anus, and gently pushing his finger inside the anus to look for the presence of any lumps or other abnormal outgrowths. This examination is termed as DRE (Digital Rectal Examination).
(3) In some cases, a physical lump may not be presented and cannot be felt by the surgeon. In such cases, to rule out the possibility, the surgeon would perform a proctoscopy. An instrument that is like a tube called a proctoscope is inserted into the anal region and checked for the presence of piles and assessing the grade of it. With this, the surgeon can pinpoint the presence of piles or other medical conditions like tumor growth, etc.
(4) The advantage of visiting a surgeon is, he is qualified to rule out other medical and surgical conditions that are causing discomfort or bleeding in the anal region. He may rightly prescribe other diagnosis methods if the medical condition is to rule out to piles.
General Treatment Procedures for Piles
Treatment for piles varies depending on the grade of the piles and also the intensity and status of bleeding.
- As a general measure, if the grade of the piles is 1 or 2, and if bleeding is not persistent and is rare, the piles specialist prescribes over-the-counter laxatives for a few days.
- In grades 2, if the bleeding is a cause to worry, Piles Surgery procedures like Banding or Sclerotherapy are recommended.
- If the grade is 3 or 4 and the bleeding is also a cause of worry, the pile's surgery type recommended is Haemorrhoidectomy.
General Recommendations for Managing Piles
As part of managing piles, the piles specialist would recommend the patient to do the following,
- Include more fiber in the diet.
- Taking steps to reduce their weight (obesity)
- Being physically active.
Piles Surgeries
A surgeon generally recommends surgery for piles or hemorrhoids is when conservative Piles Treatment methods like home remedies, diet, laxatives have failed. The surgeon will also recommend surgery when complications of piles have come. Based on the grade of piles or hemorrhoids there are different types of piles surgery that piles surgeons recommend. The three common types of piles surgery are Rubber Band Ligation (Banding), Sclerotherapy, and Hemorrhoidectomy.
Surgery type for piles varies depending on the grade of the piles and also the intensity and status of bleeding.
- If the piles is of grade 2 and if there is bleeding that is worrying, piles surgery procedures like Rubber Band Ligation (also called Rubber Band Ligation or Haemorrhoid Banding) or Sclerotherapy are recommended. Both these surgery types are only for internal piles.
- For grade 3 or 4 piles with bleeding, the surgeon will recommend Hemorrhoidectomy.
- Generally, all prolapsed piles and thrombosed piles require Hemorrhoidectomy surgery.
Types of Piles Surgeries
Rubber Band Ligation
Who is Eligible for Rubber Band Ligation?
For most of the patients with Haemorrhoids or piles, and the grade is 2 and if the piles are above the dentate line, they can be treated by the above Rubber Band Ligation method. This surgical procedure is an outpatient method.
A brief about Rubber Band Ligation Surgical Procedure
- Topical anesthesia is applied in the anal/rectal region if the number of prolapsed or thrombosed piles or the tuft of veins is minimal in number.
- Sometimes if the piles number is many, the piles surgeon might decide to do banding in phases and the procedure may be performed in multiple sittings.
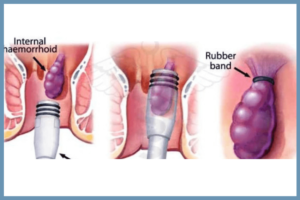
- The piles surgeon then inserts an anoscope into your rectal region and reaches out to the piles. An anoscope is a small tube with a light at the end which is very similar to an endoscope but a miniature one. After this, the piles surgeon inserts a tool called a ligator inside through the anoscope.
- A ligator is a tool that helps in placing very small rubber bands, usually a few millimeters wide, to the base of the hemorrhoids.
How Rubber Band Ligation surgery for piles helps to treat Haemorrhoids?
- The small rubber bands placed to the base of the vein tufts cuts the blood supply to the piles.
- The hemorrhoids then dry without blood supply and then falls off along with the rubber band on its own. Usually, they fall and pass out along with the stools.
- The time take for the hemorrhoids to dry after the rubber bands have been placed may take anywhere from one to two weeks.
What it feels like after undergoing Rubber Band Ligation surgery for piles?
- Slight discomfort can be felt in the bottom region after the procedure. This discomfort might last for a few days.
- Passing gas often is normal after the procedure.
- Slight bleeding might occur when going to the toilet. This is not a cause to worry as it is normal.
- Feeling constipated for a few days is also normal after undergoing this procedure.
What are the advantages of Rubber Band Ligation Surgery for Piles?
- It is generally an outpatient procedure and does not require any hospitalization. The entire treatment time is dependant on the number of rubber bands that are required to be placed.
- The chances of recurrence of hemorrhoids are less in this procedure.
Sclerotherapy
Who is Eligible for Sclerotherapy?
Patients with grade 2 Haemorrhoids or piles are eligible for sclerotherapy surgical procedures. The eligibility is almost equal for both the Rubber Band Ligation method and Sclerotherapy. This surgical procedure involved in Sclerotherapy is also an outpatient method. The surgeon prefers banding to sclerotherapy these days.
A brief about Sclerotherapy Surgical Procedure
- This procedure involves injecting a chemical solution into the vein tufts that are causing the piles.
- This chemical basically scars the veins causing the blood vessel of the piles to shrink.
- Even smaller tufts of piles can be treated using sclerotherapy.
How Sclerotherapy surgery for piles helps to treat Haemorrhoids?
- The shrunk piles basically dry up and end up falling and passing out along with the stools.
- The time take for the hemorrhoids to dry after the sclerotherapy procedure has been carried out may take anywhere from four to six weeks.
What it feels like after undergoing Sclerotherapy surgery for piles?
- Mild pain might be there after the procedure. This discomfort and pain might last for a few days and it is quite common.
- Slight bleeding for few days after the procedure is also common.
What are the advantages of Sclerotherapy Surgery for Piles?
- It is also an outpatient procedure and does not require any hospitalization.
- No anesthesia
- The procedure comes in handy for patients with more number of prolapsed piles are found and when they are not large enough for rubber band ligation.
Haemorrhoidectomy
Who is Eligible for Haemorrhoidectomy?
Patients with grade 3 and 4 Haemorrhoids or piles are eligible for Haemorrhoidectomy surgical procedure. In other words, it is a surgery for severe piles. This surgical procedure is recommended only when the piles are large and cannot be treated by rubber band ligation and sclerotherapy methods.
How to prepare for Haemorrhoidectomy Surgical Procedure?
- This procedure is not an outpatient procedure. It is a full-blown surgical procedure and requires anesthesia to be administered before the surgery. It can also be done as a daycare procedure.
- Your piles surgeon will fix the date for the surgery and usually ask you to avoid food for a few hours before the surgery.
- Your piles surgeon will also review any medications you are taking for any other illness and may instruct you to stop certain medications if need be for the recommended number of days, both before and after the piles surgery. Usually, it is the blood-thinning medications that need to be stopped before any surgery. Your piles surgeon would know better and will advise you appropriately.
A brief about Haemorrhoidectomy Surgical Procedure
- The procedure involves opening the anus and incising the hemorrhoids out.
- Off late more surgeons use sophisticated medical instruments that can perfectly shave off the hemorrhoid tissues from the anal region.
How Haemorrhoidectomy surgery for piles helps to treat Haemorrhoids?
- Since it directly incises the hemorrhoids causing veins, they completely remove them with the surgery.
What it feels like after undergoing Haemorrhoidectomy surgery for piles?
- Pain is a factor after the surgery as the entire hemorrhoid tissues have been completely removed. But this is not a cause to worry because your piles surgeon will prescribe effective pain killers.
- The pain might last a few weeks after the haemorrhoidectomy procedure which is anyway normal.
What are the advantages of Haemorrhoidectomy Surgery for Piles?
- The probability of hemorrhoids returning or recurrence is very less compared to other methods of piles surgery.
- This procedure comes in handy for people with severe piles condition.
Dr Maran on Piles Surgery
Dr Maran, a piles specialist in Chennai, has been routinely performing Piles surgery in Chennai for many years. As one of the best doctor for piles treatment in Chennai, he tells us that Rubber Band Ligation or Banding is used for Hemorrhoids that are moderate and Haemorrhoidectomy surgical procedure is used for people with severe piles condition.